PGT or Preimplantation Genetic Testing, lets you know the genetic competence of an embryo before it is transferred to the uterus.
Why should embryo’s be tested for genetic Abnormalities?
The final aim of human conception is to deliver a normal and healthy child. A normal child is a result of normal genetic makeup of the embryo. Both parents contribute half of the chromosomes (genes) and the combination of these genes determine the genetic makeup of the embryo.
Human reproduction is extremely inefficient because a fertile couple stands only 25% chance of conception in each cycle, out of which only 50% are capable of developing to term. Among the many factors that contribute to high rate of loss of embryo, one of the most significant reason is Chromosomal Abnormality (Aneuploidy or Numerical Error in Chromosome numbers to be specific). To know more about types of Chromosomal Abnormalities, please read out Blog on the same.
What we need to know is that numerical errors in early embryonic development is the most common cause of early pregnancy loss and surmounts to approximately 60% of all natural conception. Among the Aneuploidies, Trisomy 21 (or Down’s Syndrome) or extra chromosome in the 21st Pair makes it the Most Common Chromosomal abnormality resulting appx 64% of all Aneuploidy.
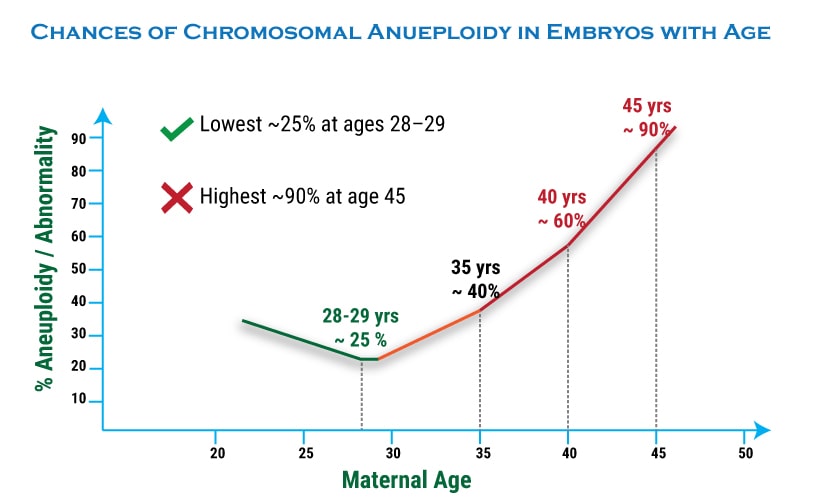
It is important to know that incidence of Chromosomal Aneuploidies are directly related to the Maternal Age and increases exponentially after 35 and as high as 80% at the age 42.
WHAT TYPES OF GENETIC ABNORMALITIES CAN PGT DETECT?
To know more about genetic abnormalities in general, please read our BLOG on the same.
Pre Implantation Genetic Testing is broadly classified into three types of testing:
PGT-A – PGT for Aneuploidies (earlier known as PGS)
Pre-Implantation Genetic Testing for Aneuploidies is used to screen for numerical errors (defined as Aneuploidies) in all 23 pairs of chromosomes.
The test will only report Gain or Loss of chromosome numbers. PGT-A is used to deselect the abnormal embryo’s and hence acts as a selection tool by helping us choose the embryo that will most likely result in a successful pregnancy.
When should patient’s be counseled for PGT-A
Advance Maternal Age of 35 or above with one of the co-existing factors:
- Severe Male factor Infertility including Azoospermia, OATS etc
- Recurrent Implantation Failure
- Multiple Pregnancy losses
- Previous history of a live born child or pregnancy with Aneuploidy

PGT- SR for Structural Rearrangements
Genetic test used to screen for Structural Rearrangements of chromosomes i.e. gain or loss of genetic material due to Inversions, Translocations or Deletions.
About 1 in 1000 people in general population have Translocation error (i.e. exchange of genetic material between two chromosomes). It is estimated that about 70% of embryos that are generated by a parent with Reciprocal Translocation are abnormal. Hence it becomes increasingly important to test the embryo’s generated by parents of known genetic Structural Rearrangements. (e.g. Reciprocal Translocation, Robertsonian Translocation, Insertions, Deletion etc)
When should patient’s be counseled for PGT-SR
It is important to know that individuals who present Translocation Errors are typically healthy and show no signs of any developmental delays, hence they are most often completely unaware of their condition. Such patients usually present with multiple pregnancy losses or recurrent implantation failure. It is advisable to get the Karyotyping of both partners done to rule out genetic reasons.
If the Karyotyping result shows any Structural Rearrangement like Reciprocal Translocation or Robertsonian’s Translocation, it becomes imperative to counsel the patients about their chances of having a genetically normal baby. The patient should be offered PGT-SR with IVF cycle depending on factors like Antral follicle count, economic status etc.
PGT-M – PGT for Monogenic Disorders (earlier known as PGD)
Globally the occurrence of Single gene Inherited diseases at birth is approximately 1%
Here is a list of the most commonly inherited Single Gene Disorders:
- Thalassaemia (Both Alpha and Beta Thalassaemia)
- Sickle cell Anemia
- Haemophilia
- Cystic Fibrosis
- Tay sachs disease
- Fragile X syndrome
- Huntington’s disease
- BRCA mutations (genes for Cancer predisposition)
Monogenic disorders are caused by defect in a single gene (mono) that could have been passed by either of the parent or could have been developed during Embryo development.
When should patients be counseled for PGT-M?
Following patients should be counseled to undergo PGT-M (PGT for Monogenic disorders)
- Suffer from single gene disorder
- Or have a family history of these disorders
- Or have a child who is already affected by these genetic disorders
PGT-M helps significantly decrease the chance of having a child with an inherited genetic disorder because patients can choose to transfer only those embryos that are genetically normal.
Future of PGT
Availability of better embryo culture media, improved cryopreservation media and protocol along with safe embryo biopsy technique as well as accurate genetic testing methods have contributed immensely towards the efficacy and accuracy PGT in the last decade. Availability of better technology, tools and constant innovation and advancement is constantly finding novel ways making pregnancy safe and affordable. The next innovation on the cards is niPGT (non-invasive PGT is a technique for testing the genetic makeup of embryo without embryo biopsy by analyzing the culture medium around the embryos) which we all are waiting for.
Concluding Remarks
Technology should not always be used just because it is available.
Along with many benefits of PGT, we also see many serious disadvantages of the technique. High degree of invasiveness of the procedure and cost being the top on the list. PGT-A should be offered very conservatively, PGT-M for monogenic disorders like Thallasemia, Sickle Cell etc seem to be the most logical indication for PGT where it makes absolute sense.
Genetic Counseling
If you think you need genetic counseling for your case, do drop in a message with case history, we will be glad to help!
WHATSAPP FOR GENETIC COUNSELING