Treatment for Azoospermia
Azoospermia is defined as the absence of spermatozoa in the ejaculate or simply absence of sperms in semen or when no sperm is found in semen. Often patients want to know if Azoospermia is same as Nil Sperm. Nil sperm is the colloquial term used for Azoospermia in most rural parts of India. Azoospermia accounts for about 20% of all cases of male infertility and in 10-20 % of abnormal Semen Reports.How do I know my Sperm Count ?
The easiest way to know your sperm count is to undergo a Semen Analysis test. You do not need any written prescription from an Infertility Specialist to undergo a semen analysis test at any pathology. Routine Semen analysis test at Indore can be done at any standard pathology, however if you wish for Advanced Semen Analysis that uses special microscope to view the sperm morphology you should get it done from an IVF clinic . Our IVF Clinic in Indore uses Phase Contrast Microscope which enhances the three dimensional image of the sperm so that it is easy to identify the morphology of the sperm.My semen analysis report mentions Azoospermia ? What does that mean ?
When no sperms are seen in the semen sample provided for testing even after centrifugation of the sample, the report mentions Azoospermia. Good andrology labs always confirm the absence of sperm by centrifuging (spinning at high speed) the entire sample and checking each drop to confirm the diagnosis. An IVF specialist usually will ask the patient to test their semen sample after a gap of few days again to confirm if the second sample also shows absence of sperm.
What is most common cause of Azoospermia ?
Azoospermia or Nil Sperm in ejaculate can be caused by some of the following:
- Vasectomy – Tying the tubes as a method of male contraceptive.
- Abnormal growth of testes which could be congenital or be an effect of genetic abnormalities.
- Result of chemotherapy or radio therapy as a treatment for some form of cancer.
- Abuse of recreational drugs or narcotics may cause abnormal semen parameters. However in most cases this is reversible.
- Anatomical abnormalities that can cause absence of vas deferens – A tubular structure that carries sperms produced from the testes to the ejaculatory duct. The anatomical abnormalities could be a result of genetic mutation or genetic abnormalities.
- Genetic abnormalities like Klinefelter’s syndrome, Y Chromosome microdeletion etc. As many as 20% patients with azoospermia have chromosomal abnormalities.
- Condition called cryptorchidism, which presents with small testes , elevated LH and FSH. Such patients usually do not have any mature sperm in their ejaculate.
- Childhood infection with Mumps, testicular trauma or torsion or scrotal surgery of some sort may also result in missing sperms in semen analysis report.
These are just few of the causes of azoospermia. Till date there is no test that can report the actual cause of azoospermia in patients since it is not completely understood yet.
Can patient with Azoospermia have normal FSH ?
Yes. Patients with obstructive Azoospermia, do have normal level of FSH.
How is Azoospermia diagnosed ?
The preliminary diagnosis of azoospermia needs to be followed by:
- Confirming the diagnosis of Azoospermia through repeat semen sample.
- Determining whether it is Obstructive or Non-Obstructive
- Assessing for the presence of correctable causes
- Offering appropriate ART methods for conception like ICSI and TESA
As a standard practice, one single report of Azoospermia cannot be considered conclusive and semen analysis has to be repeated after a few days. An abstinence of 2-3 days is recommended before repeating the test. Your IVF doctor will recommend you the appropriate abstinence and ask to get evaluated again.
The World Health Organization has given guidelines for performing semen analysis before labeling a sample as Azoospermic. Please ensure these guidelines have been followed at the lab where this test is being performed. The guideline is available here for the purpose of reference: World Health Organization. WHO laboratory manual for the examining and Processing of Human Semen, 6th Edition.
Evaluating and Treating Zero Sperm in Males (Azoospermia) is a necessary step in order to decide the course of IVF treatment. In case it is confirmed that the case is of non obstructive azoospermia, patient can be counseled to opt for Donor sperms along with IVF treatment.

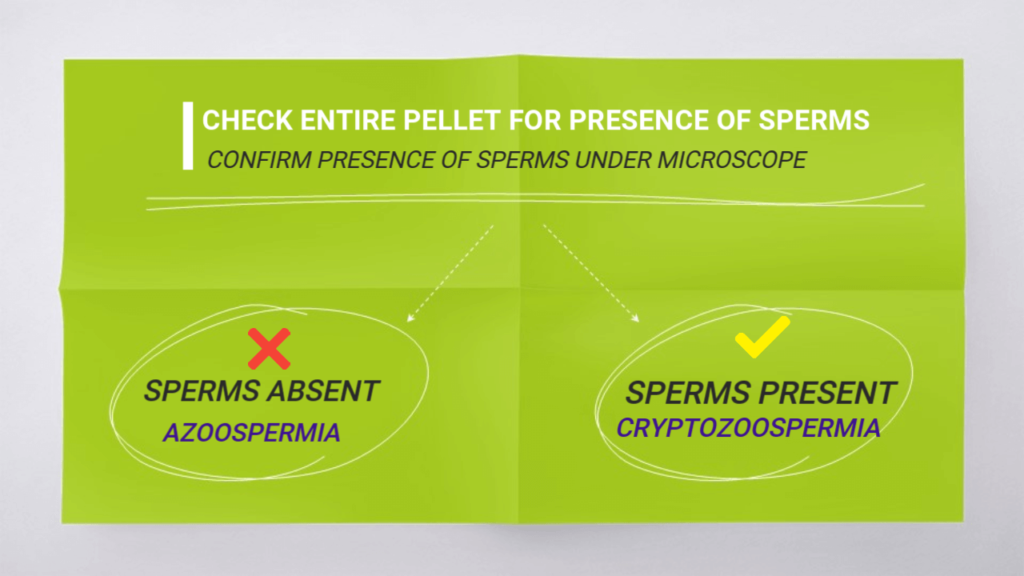
What is the difference between Cryptozoospermia and Azoospermia ?
During the analysis of the semen sample where no sperms were seen initially, the lab technician will centrifuge the sample and test each drop of the sample to confirm presence of occasional sperms. If a few sperms are found in the centrifuged pellet of the sample, then such samples are reported as cases of Cryptozoospermia.
However if no sperms are seen even in the centrifuged sample, the diagnosis of Azoospermia is confirmed.
What is the difference between Non Obstructive Azoospermia Vs Obstructive Azoospermia (OA) ?
In cases where sperms are being produced however are not delivered in the semen, the type of azoospermia is termed as obstructive azoospermia.
Cases where the mechanism of spermatogenesis is affected, meaning, no sperms are being produced in the testes, such cases are termed as non obstructive azoospermia.
Presence or absence of fructose, level of hormones like FSH, LH and testoesterone , size of testes and finding of scrotal USG along with patients history helps an IVF specialist or Male Fertility specialist to identify if the azoospermia is obstructive or non obstructive.
Does Obstructive Azoospermia mean that there is hope for sperm recovery ?
Obstructive Azoospermia means that sperms are being produced in the testes but fail to be delivered in semen. In Obstructive Azoospermia, generally the testes are normal sized and FSH levels are normal. The semen sample typically does not contain Fructose ( Lab Report shows Fructose Negative).
Obstructive Azoospermia with normal hormonal profile has a high chance of sperm recovery by process of surgical sperm retrieval like TESA.
Treating Azoospermia with Intracytoplasmic Sperm Injection is a possibility if it is a case of obstructive azoospermia.
Azoospermia treatment cost in Indore Infertility Clinic has always been affordable.
What does Fructose test mean ?
The Fructose Test determines if fructose is present in the semen sample. If fructose is not present in the semen sample then it is a case of Fructose Negative Azoospermia or Obstructive Azoospermia.
Obstructive Azoospermia is very easy to treat with either surgical reconstruction or surgical sperm retrieval using procedures such as TESA, TESE and then performing ICSI and IVF.
Obstructive Azoospermia has very good prognosis and pregnancy rates.
What is Fructose Positive Azoospermia ? Is it same as Non-Obstructive Azoospermia ?
Azoospermic samples that are fructose positive may be case of Non obstructive azoospermia.
In non-obstructive azoospermia, there are chances that sperms are not being produced in the testes as a result they are absent in the ejaculate. In this type, size of testes is usually reduced and FSH levels are either very high or very low. Such samples usually have normal volume and contain fructose (Lab report shows fructose positive).
Non-Obstructive Azoospermia can be because of multiple causes ranging from genetic to infectious to hormonal reasons. It is therefore important to diagnose the cause by carrying out further investigations like Hormone Studies (Blood Investigation), Ultrasound etc.
The prognosis of non-obstructive azoospermia will depend on the cause of Azoospermia.
What is the treatment of Azoospermia?
Depends on the type of Azoospermia, if it is a case of Obstructive Azoospermia, sperms can be surgically retrieved by procedure called TESA in order to achieve parenthood.
TESA or Testicular Aspiration of Sperm is a method in which sperms are surgically retrieved from the testes.
These sperms are then processed in lab and used with ICSI procedure to fertilize oocytes.
Men with Azoospermia can father a child using this procedure successfully.
It is a minimally invasive procedure and performed under mild sedation. To know more read our Blog on the same.
Who is the best doctor for azoospermia treatment or Nil Sperm treatment ?
IVF Specialists who are Male Infertility Specialist are called Andrologist. However, Infertility and the best IVF Specialists are trained in reproductive medicine and can give preliminary treatment for men dealing with Azoospermia or Nil sperm.
Men often find it difficult to talk with female gynecologist to discuss their problem. Our reproductive medicine specialist Dr. Gajendra Singh Tomar is the best IVF specialist in Indore and is a very empathetic listener, which makes treatment for both partners very easy.
Men who undergo azoospermia treatment at Indore Infertility Clinic, usually are very satisfied with their consultation with Dr. Gajendra Singh Tomar.
What is Azoospermia treatment cost ?
The cost of azoospermia treatment in Indore Infertility Clinic is typically around 25 thousand over and above the IVF package, which includes cost of TESA.