What to do when IVF Fails
When a couple is unable to conceive after IVF ICSI treatment, it is extremely frustrating both for the couple and their Doctor.
Both the doctor and the couple should understand that in spite of everything being absolutely normal, IVF in the best of situations gives success rates in the range of 40-50%.This means that 50-60% patients will not become pregnant during an IVF cycle. This bitter pill about IVF failure is best taken before starting IVF treatment rather than after failing it.
After an IVF cycle is unsuccessful, the only thing one can do is ensure is that all the parameters required for success are in the optimum range. The three things required eventually for a successful outcome are: A Good Endometrium, a Good Sperm and a Good Oocyte resulting in a Good Embryo.
Good Grade A Embryos, Triple layered Endometrium of 8mm or more and an Easy Embryo Transfer, All that you need to do is continue doing the same. Usually it’s just a matter of TIME !!
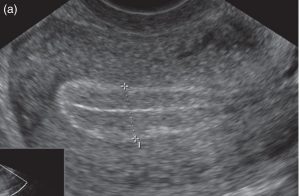
Problem with Endometrium
If endometrium is not thick enough or does not show the desired triple layer appearance on ultrasound, medicines to improve endometrium should be given. Agents like Estradiol, Aspirin, Vitamin E, Vaginal Sildenafil, L Arginine are known to support the endometrial receptivity and growth.
Apart from thickness of endometrium, a triple layered pattern is desirable.
If in spite of medicines the endometrial parameters are suboptimal, searching for other causes such as Intra Uterine Adhesions, Endometrial Infection, Tubercular Endometritis, High levels of Prolactin hormone etc. should be excluded. Usually some blood tests, endometrial sampling and hysteroscopy may be required if any of these abnormalities is suspected.
During a stimulation cycle, Endometrium may not be optimally receptive because of the abnormally high serum Estradiol levels. Frozen Embryo Transfer is known give better results than fresh Embryo Transfer and should be tried in such cases.
ERA or Endometrial Receptivity Assays are available nowadays but there is not a lot of evidence that suggests doing this test improves the pregnancy rates.
If in spite of all corrective measure, endometrium remains sub optimal and Implantation fails on repeated occasions, Surrogacy is one option that a couple should always consider.
Problem with Oocyte
To counter the effects of poor quality oocytes due to an increase in age, DHEAS is used for upto 8 weeks before starting the IVF cycle.
If the response to stimulation in the previous cycle was less than expected (Poor Responder), increasing the gonadotropin dose should be considered. If the response was more than expected or excessive because of PCOS, using lower doses for a prolonged period of time is recommended. Also if the number of oocytes retrieved is higher, freezing them all and transferring the embryos in a natural cycle always gives better results.
If poor oocyte numbers and quality cannot be improved, the option of oocyte donation should be discussed with your doctor.
Problem with Sperm
Semen showing very poor count and motility often gives very poor fertilization rate. To avoid this, anti-oxidants should be taken well before commencing IVF-ICSI. Performing DNA Fragmentation Index (DFI) also helps in estimating the damage to the DNA of the sperm. An Andrologists’ opinion for improving semen parameters should always be sought for suggesting the correct line of treatment to get the best possible sperms.
Sperm selection and a well performed ICSI usually gives good fertilization rates.
Sperm Donation is very rarely required nowadays and is done only when surgical sperm retrieval does not yield any mature spermatozoa.
Problem with Embryo
If previous Embryo Transfers were done on day 3, doing a day 5 Transfer or Blastocyst Transfer is always advisable. If we are unable to culture embryos upto day 5, considering all laboratory parameters are perfect, we can assume that the problem is with the embryo and then take further action accordingly. This is especially true if the multiple Embryo Transfers were done on day 3 and now Blastocyst culture has failed.
A combination of culture up till Blastocyst stage, vitrification and Embryo Transfer in subsequent cycle will give the best possible results. This is because in a stimulated cycle, high levels of circulating estrogen hormone impair implantation. In a natural unstimulated cycle, implantation rates are as high as 70%.
Immunological Factors and Immune Therapy
Immune Testing in multiple IVF failures is in vogue nowadays and there are a number of immune markers like ANA, APA, NKA, TJP, Anti DNA AntiHistone Antibodies that are commonly performed in order to find the answer of the most sought after question – Why did my IVF Fail ?
The truth is that these tests are poorly standardized and interpretation is very difficult because of the variations in reporting. Secondly, many of these tests come back as abnormal in perfectly fine, fertile women too. There is also no evidence or study that proves that Immune therapy improves pregnancy rates.
So In short, we as a routine do not offer any immunological tests and do not give immune therapy at present. If there is compelling evidence in the future, we will definitely reconsider our position on this issue.
Problem with the process of Embryo Transfer
No matter how good the Embryo and Endometrium are, If the procedure of Embryo Transfer is not smooth, implantation is very unlikely to occur. Sometimes Cervical Stenosis, Acute Angulations of the uterus may cause difficult transfers. Doing a trial transfer before starting the cycle and resolving all issues before the actual procedure are advisable.
Conclusion
Asking for a second opinion and a fresh start never does any harm. For a second opinion, please feel free to visit us or contact us using our Online Consultation Platform.
If all parameters are fine, Just keep on trying. The fact is that all IVF clinics have patients who conceive after multiple attempts without any change in the protocol whatsoever.
This just means that at times, It’s Just a Matter of TIME
So be Positive, be Patient and be Persistent.