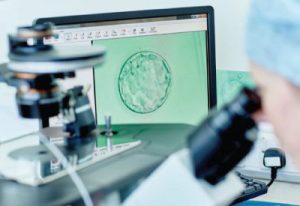
What is ICSI?
Intra-cytoplasmic sperm injection ( ICSI ) involves injecting a single sperm directly into an egg in order to fertilize it. The fertilized egg (embryo) is then transferred to the woman’s womb just like regular IVF.
How is ICSI Procedure Performed?
ICSI is done as a part of IVF. Since ICSI is done in the lab, your IVF – ICSI treatment won’t seem much different than an IVF treatment without ICSI. However for the male partner, ‘how’ the sperms are extracted might be different.
For women
For a female partner, the steps are similar to IVF Procedure.
For men
Just like regular IVF, the Male partner will be asked to produce semen sample on the same day as the egg retrieval. The semen will be analyzed under microscope and usually the best sperm will be extracted. However if the semen analysis shows that the sample hardly has any viable sperms, the Male partner may have to undergo some procedures for extraction of sperms.
Depending on the cause of male infertility Sperms can be extracted/collected from:
- The epididymis (a narrow tube inside the scrotum, where sperm are stored and matured) using a type of fine syringe. This process is known as ‘percutaneous epididymal sperm aspiration’ or PESA.
- OR from the testicles, using a process known as ‘testicular sperm aspiration’ or TESA.
- OR from tiny quantities of testicular tissues which are removed after testicular biopsy. This procedure is called ‘testicular sperm extraction’ or TESE.
After retrieval of sperm,an embryologist will place the eggs in a special culture, and using a microscope and tiny needle, a single sperm will be injected into an egg. This will be done for each egg retrieved. This does not automatically mean that the egg is fertilized, but ICSI now gives an opportunity for that complex process to commence.
ICSI is not a guarantee that Fertilization will take place
Subsequently one to three of the best quality embryos are transferred to the womb just like a regular IVF Cycle
When is ICSI recommended?
ICSI is an advanced version of artificial reproductive techniques. It helps in achieving fertilization even in extreme male factor infertility and certain fertilization failure cases. Here are some common reasons to go for an ICSI:
Male Factor Infertility:
ICSI helps in achieving fertilization in cases of severe male factor infertility.
- Very low sperm count.
- High percentage of abnormally shaped sperm.
- Poor motility of sperms.
- Ejaculatory problems in the male partner. In such cases, the man can have problems getting an erection and ejaculation.
Frozen Semen Sample:
In some cases, a frozen semen sample might be needed. The process of freezing and later thawing the sample might cause damage to the sperms. ICSI can help in such cases in achieving fertilization.
Sperm Retrieved by Surgical Methods:
Whenever a man has obstructive azoospermia (no sperms seen in the semen, because of obstruction in the path of sperm travel), ICSI an help in achieving fertilization. The sperms are retrieved by surgical methods in these cases. But these sperms sometimes have abnormalities like motility problems or more abnormal forms than normal. Thus, ICSI is useful in such cases.
Previous IVF Failure:
If a previous IVF did not result in any embryo formation, then ICSI can be offered to the couple to ensure a better chance at fertilization and embryo formation. Thus, increasing the overall chance of a successful pregnancy.
Diminished Ovarian Reserve:
In cases where the eggs retrieved are expected to be are very less in number, then ICSI can help in getting more embryos out of the cycle. ICSI increases the chances of fertilization, and improves the outcome of the treatment cycle.
If you have been advised ICSI as an option, you can discuss with your infertility doctor about why it has been advised and how it can help you in getting pregnant.
How is ICSI different from conventional IVF?
ICSI and IVF are both advanced reproductive techniques used to achieve pregnancy in infertile couples. They are almost similar, but they differ in the technique of achieving fertilization, read on to get an overview.
Pros of using ICSI:
- Better fertilization, more embryos formed: ICSI gives better fertilization results, so the chance of embryo formation can be increased. This is helpful in male infertility and female infertility causes like diminished ovarian reserve.
Cons of using ICSI:
- Costlier than IVF: Additional equipment and usage of lab facilities in ICSI increases its cost compared to IVF.
- Possible damage to gametes: The gametes (sperm and egg) can be damaged during ICSI because they are manipulated using micro instruments. This could also lead to an effect on the embryo which is formed.
Pros of IVF:
- Less damage to gametes: The eggs are fertilized by sperms naturally, without any instrumentation, and hence IVF does not damage the gametes or the embryo.
- More affordable than ICSI: Usually more affordable than ICSI.
Cons of IVF:
- Less chance of fertilization in some cases: In cases of severe semen abnormalities, like extremely low sperm count or sperm motility, fertilization chances are less.
You should discuss all the pros and cons with your fertility specialist when going for an artificial reproductive technique to get pregnant. They will guide you in making the right decision according to your health condition and needs.
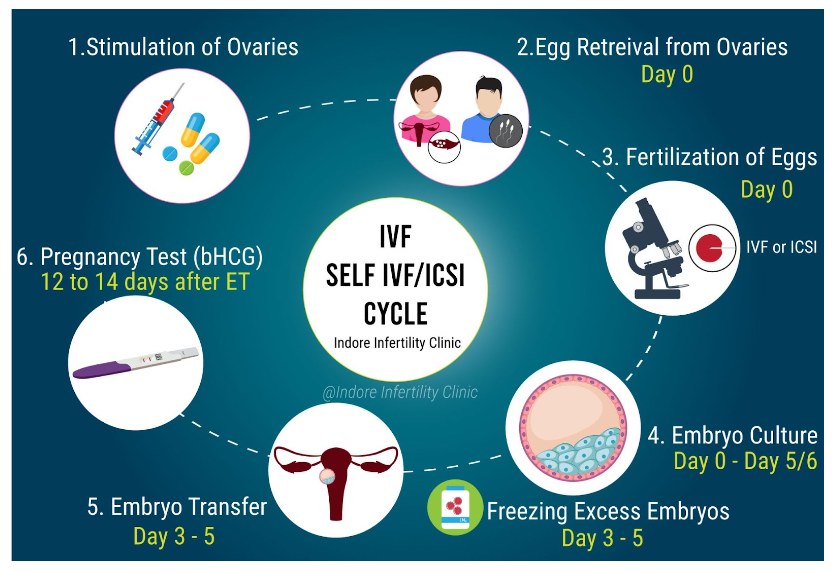
Step-by-step guide to the ICSI procedure
ICSI is almost similar to a conventional IVF procedure, except for the fertilization part. Here’s a step-by-step guide to the ICSI (Intracytoplasmic Sperm Injection) procedure:
- Ovarian Stimulation and Oocyte Pickup: This part is just like a normal IVF protocol. The eggs in the woman’s ovary are stimulated by hormonal injections. Their growth is monitored by sonography and eventually they are picked up by a fine needle. The pickup procedure is done under sedation.
- Semen Collection/Sperm Retrieval: The sperms are obtained from the male. The sperms can be obtained by processing a sample after a fresh ejaculate, or sometimes a cryopreserved (frozen) sample. In cases of obstructive azoospermia sperm can be retrieved by testicular biopsy. This procedure is done under anaesthesia.
- Sperm Preparation: To select the best quality sperms and clear the semen sample of any unwanted substances, semen sample is prepared in the lab.
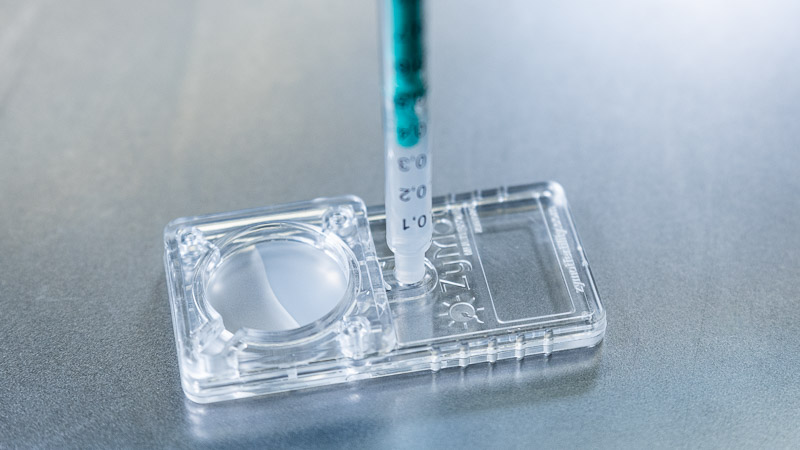
- Sperm Injection into the Egg (ICSI): A single sperm is carefully selected and injected into good quality mature egg retrieved from the woman using a specialized microscope and equipment. This is done for each of the eggs obtained from the ovaries. This process is the key step which differentiates ICSI from IVF. This process increases the chances of fertilization, but it does not guarantee that it will happen.
- Confirmation of Fertilization: The eggs injected with sperms are then checked for confirmation of fertilization. It is done by checking for the changes expected in the egg after fertilization under a microscope.
- Embryo Culture: The embryo formed out of the fertilization of egg by the injected sperm is allowed to develop further in the lab. This is called embryo culture.
- Embryo Transfer: After culturing the embryos in the lab, the best ones are then chosen to be transferred into the uterus of the woman. The number of embryos to be transferred depends on the particular couple and their needs. It can be done on day 3 or day 5 of fertilization, based on the individual case.
- Cryopreservation of the Embryos: If extra embryos are formed, they can be cryopreserved (stored in the lab after freezing). This can be helpful in either implantation failure or in case of future fertility desire.
What is the success Rate for ICSI?
ICSI can give a higher fertilization response than a conventional IVF. Success rate is quoted to be between 70-80% in different scientific literatures. The success rates of ICSI can vary depending on various factors, including the age of the woman, the quality of the sperm and eggs, and the expertise of the fertility clinic. Eventually, the purpose of an ICSI procedure is to give a successful pregnancy, and a live born baby. Thus, multiple factors come into play.
Factors Affecting the Success of ICSI:
- Age of the Woman and Egg Quality: It is one of the prime factors which affect any fertility treatment. Advanced age of woman leads to poor quality of eggs, as well as smaller number of eggs available for fertilization.
- Semen parameters: Semen parameters like sperm count, sperm shape and sperm motility can significantly impact the results of any ART procedure, including ICSI.
- Embryo Quality: Good quality embryos are related to better chances of implantation, and vice versa. Hence, choosing the best quality embryos to transfer is a key determinant in the outcome of treatment.
- Underlying Causes of Infertility: If there are other conditions which create a hostile environment for implantation of the embryo in the uterus, then also the response would be inadequate.
- Uterine factors: Conditions like suboptimal endometrial thickness (thickness of the lining of the womb), or endometrial polyps (growth in the lining of the womb), or reduced blood flow into the uterus can also reduce the chances of implantation. It is essential to address them before going for an embryo transfer to ensure good results.
- Lifestyle Factors: Smoking, excessive alcohol consumption, and obesity are additional factors which can reduce the chances of implantation of an embryo. All steps should be taken before an embryo transfer to cut back on any habits which can impair chances of a successful pregnancy. Also, women should try and reduce weight and try to be as close as possible to the healthy BMI range of 18-24 Kg/m2.
- Experience of the Embryologist: Since it is a procedure handled by embryologists, their expertise and experience can make a huge difference. The more experienced they are with ICSI, better should be the results.
The above list will help you understand what role each person, or factor plays in the success of an ICSI procedure, and how you can ensure that you get the best outcome out of your treatment. It also helps you set a realistic goal when it comes to treatment results.
What are the advantages of ICSI?
- As compared to IVF, ICSI has better fertilization rates. This allows for more embryo’s to be formed and therefore increases the chances of cryopreservation of embryo’s.
- ICSI may give you and your partner a chance of conceiving your genetic child when other options are closed to you.
- If your partner is too anxious to ejaculate on the day of egg collection for standard IVF, sperm can instead be extracted for ICSI. This is usually overcome by cryopreserving a semen sample before starting the IVF cycle.
- ICSI can also be used to help couples with unexplained infertility. As ICSI and IVF pregnancy rates are very similar and ICSI leaves little scope for the unknown.
What are the Risks or Side Effects of using ICSI procedure ?
All the risks and side effects associated with IVF are also associated with ICSI.
As ICSI is more invasive and requires more handling than standard IVF insemination techniques, there is a small chance (<1%) that the egg may be damaged during the procedure – resulting in a non-viable egg.
Thousands of children have been born around the world as a result of ICSI. Till date, there is no convincing evidence that the incidence of birth defects is any different with ICSI or IVF as compared to those children born to other parents of similar age and health.
Concerns with ICSI:
- It is more invasive than IVF
- Can damage the egg during manipulation, leading to a non-viable egg in < 1% cases
What is the cost of ICSI treatment ? Why is it more expensive than normal IVF ?
In India, the cost of a single cycle of ICSI can range from approximately ₹1,50,000 to ₹2,50,000 INR. This usually depends on the location of the clinic and the services offered. This usually includes the ovarian stimulation, oocyte pickup, ICSI and embryo transfer. Additional costs may be added if sperms are retrieved by any surgical method, or sperms had to be prepared by special methods in specific conditions.
Preparing for an ICSI cycle: Diet, lifestyle, and medications
Preparing for an ICSI cycle is no different than an IVF cycle. Ideally both partners should try and maintain a healthy lifestyle, quit smoking and limit alcohol. Any substance used for abuse should be stopped and if obesity is a concern, then you should take relevant steps to reduce weight. Your fertility specialist will also prescribe you some supplements to improve the quality of oocytes in women and sperms in men.
Dietary advice:
- Fresh fruits, berries, nuts, leafy vegetables (read our blog about azoospermia on specific dietary advice on improving semen parameters)
- Avoid junk food, trans fats, preserved food
- Keep yourself well hydrated
Lifestyle changes:
- Maintain a healthy BMI
- Avoid alcohol, stop smoking and any substance abused
- Avoid physical and mental stress
Medications:
- If you are on any prescription medicines already for other conditions like – thyroid disorders, diabetes, high blood pressure etc, you should visit the prescribing doctor for a review and pregnancy safety check.
- It is important that you continue such treatment to keep the concerned condition under control.
- Women who are undergoing an IVF/ICSI treatment should get their prescription medicines reviewed to check for safety for the intended pregnancy.
- Your fertility doctor might prescribe you antioxidants and supplements to ensure that you have good quality eggs and sperms when you undergo this treatment.
- Ensure that you comply with any medicines and injections started as a part of your IVF/ICSI treatment.
By following the above mentioned steps, you can play a significant part in your treatment and improve your chances of success.

Male infertility factors suitable for ICSI:
ICSI is similar in all the cases where fertilization is difficult because of abnormality in the sperms. When there are a reduced number of healthy sperms, which can reach for the egg and fertilize it, ICSI is used to overcome that hurdle. Following are common male infertility factors, in which ICSI is very useful.
- Low Sperm Count (Oligozoospermia) – less than 39 million per ejaculate or 16 million per ml.
- Reduced Sperm Motility (Asthenozoospermia) – less than 42% motile sperms (progressive and non-progressive movement included) seen.
- Reduced Number of Normal Sperms (Teratozoospermia) – less than 4% normal forms seen.
- Reduced Number of Live Sperms – less than 54% live sperms seen.
- In cases of Obstructive Azoospermia (nil sperm because of obstruction) and Surgically Retrieved Sperms. Surgically retrieved sperms usually have these above problems, and need selection of best sperm for fertilization.
If you have any of these findings in your semen report, your fertility doctor might advise you to go for an ICSI procedure.
Latest Advancements in ICSI Technology:
The advances in techniques and innovations have refined ICSI. Following are the latest advancements in the ICSI technology:
Advanced Sperm Selection Techniques
- PICSI (Physiological ICSI): A substance called hyaluronic acid is used to select the best quality sperms. Hyaluronic acid is normally found in the female reproductive tract, and hence it is called physiological (like natural process in the body). The sperms which are selected by this method are then used to do ICSI.
- IMSI (Intracytoplasmic Morphologically Selected Sperm Injection): This is a further advancement in the ICSI procedure. Sperm samples are examined under very high-power microscope. This enables the embryologist to identify defects in the sperm head, which are not normally identified. The selected best quality sperms are then used for ICSI.
FAQ's
In IVF, the final step of fertilization happens naturally by penetration of the sperm into the egg.
In ICSI, the sperm is directly injected into the egg to assist in fertilization.
Rest all steps are almost same.
No, ICSI is not recommended for everyone. It is advised in severe male factor infertility like low sperm count, or motility, abnormal forms of sperms, and also in cases of surgically retrieved sperms. It is also useful in unexplained infertility and when small number of oocytes are retrieved because of diminished ovarian reserve.
The success rates of ICSI are around 70-80%.
There is a small chance (<1%) of damage to the egg during manipulation, it can lead to a non-viable egg. Apart from this, the risks of ovarian stimulation, ovum pickup and embryo transfer are the same as a conventional IVF.
A single cycle of ICSI can cost between ₹1,50,000 to ₹2,50,000 INR in different parts of the country.
Yes, ICSI can be used for non-male factor infertility. It is useful in where previous IVF was a failure and in cases where very small number of oocytes could be retrieved.
ICSI is a method of fertilization and should be used for cases where conventional IVF cannot be done. Alternative to ICSI could be replacement of the defected male gamete by Sperm Donor Program.
The decision about how many embryos to transfer depends on many factors like:
- Age of the woman
- Number of top-quality embryos formed
- Desire of the intending couple (after explaining all potential risks)
One or two embryos can be transferred based on these factors.
Following can be done with the excess embryos formed after ICSI:
- Cryopreservation: This can help the couple attempt more embryo transfers, in case of failure.
- Donating for research: the couple can donate the embryo for research to the embryology lab.
- Discard: If none of the above is an option, then, embryos can be discarded also.
The lifestyle changes recommended before ICSI are same as the conventional IVF procedure, they include:
- Take a healthy balanced diet
- Avoid junk food
- Keep yourself well hydrated
- Maintain a healthy BMI
- Avoid alcohol, stop smoking and any substance abused
- Avoid physical and mental stress
Take the pre pregnancy vitamins and supplements advised by your fertility specialist.
The time taken for an ICSI depends on how many oocytes were retrieved during the pickup. In an average cycle, usually 10-12 oocytes are picked up. For a single oocyte sperm injection, it takes 30-40 seconds. It can take approximately 20-25 minutes for the entire ICSI procedure, including sperm immobilization and the sperm injection.
Yes, ICSI procedure requires expertise in handling gametes (eggs and sperms), and using micromanipulation techniques. This is achieved only after advanced training and experience.
Yes, it can be used in same-sex couples and single parents. It has no restriction for use in single parents or same-sex couples.
Yes, the fertilization rate of ICSI is higher than conventional IVF in certain cases. During ICSI the sperm is directly injected into the egg, overcoming almost all barriers to fertilization.
If no viable sperms are available for ICSI, then alternative options should be discussed like:
- Surgical sperm retrieval like – TESE, PESA or micro-TESE
- Using donor sperm.
It takes at least 3 to 5 days to know about the number of embryos formed after ICSI.
Yes, ICSI can performed using frozen sperm or egg. In such cases the frozen gametes are thawed first, and then the rest of the procedure is same as for fresh eggs or sperms. It is useful where a semen sample is not obtained on the day of egg retrieval, or where eggs were cryopreserved (frozen) previously.
Failure of fertilization with ICSI can happen in very rare cases referred as Total Fertilization Failure. If that happens, your fertility doctor will provide you with the following options:
- Using a new sperm selection technique
- Replacing the possibly defected gamete (sperm or egg) with donor gametes
In couples who had previous IVF failure, finding out about the cause is important, as well as taking steps to get a successful result in the next attempt. Following points should be considered:
- Reason for previous failure: Information about previous IVF cycle like, the ovarian stimulation protocol, number of oocytes collected, sperm quality can help a lot in improving the treatment in further attempts.
- Embryos formed in previous cycle: If the embryos formed in previous IVF were not of good quality, then steps should be taken to optimize the results this time.
- Semen quality: Knowing whether poor quality sperms were the reason of failure, can help in improving the results. It can be done by either trying to enhance sperm quality or using donor sperms.
- Poor Quality Eggs: If the eggs of woman are not of good quality, then either medications to improve quality, or donor eggs as a last resort could be advised.
- Condition of the Endometrium (inner lining of the womb): Good condition of the endometrium is very important in implantation of the embryo. If any concerning condition is noticed in the uterine lining, it should be corrected before further embryo transfers.
- Pre-Implantation Genetic Testing (PGT) of the Embryos: If the defect is suspected in the embryos, they can be subjected to pre-implantation genetic testing, to ensure healthy embryos are used (read our blog about PGT to know more).
- Health conditions and Ongoing Treatment: If you are on any prescription medications for any condition, including thyroid diseases, diabetes etc. ensure that your disease is well controlled before next attempt at IVF/ICSI.
If you have had a previous IVF failure, get a consultation with your infertility specialist. Discuss about the potential causes and what all changes can be made to improve your treatment outcome.
The chances of having a miscarriage after ICSI are the same as a normal pregnancy or IVF conceived pregnancy. The miscarriage depends on the following factors:
- Age of the woman: Increased miscarriage rates with increased age.
- Quality of embryo transferred: poor quality embryo can lead to higher chances of miscarriage.
- Woman’s health: conditions like diabetes, thyroid abnormalities, prolactin hormone abnormalities, chronic illnesses, autoimmune conditions etc can increase miscarriage chances.
Ensuring these above concerns are in check before you plan an ICSI cycle will help reduce your chances of miscarriage. Discuss with your fertility doctor about what all factors can be changed to improve the success rates of your treatment.
Yes, the age of the female partner is the most important factor which decides the outcome of any infertility treatment. Following are the reasons it impacts the fertility treatment:
- Ovarian reserve: As the age advances, the egg reserve decreases in women. Smaller number of eggs, lead to even smaller number of embryos formed. It decreases the overall success rate of an ICSI cycle.
- Quality of eggs: The quality of the eggs also declines as a woman ages. This leads to poor fertilization and poor quality of the embryos formed.
- Condition of the Endometrium (lining of the womb): As a woman ages, the lining of the womb thins out because to reduced hormones in the body. This negatively impacts the implantation of the embryo. There could be other abnormalities also present which can impair implantation.
- Miscarriage rates: As a woman’s age increases, the chances of miscarriage increase. This further reduces the chances of a successful live birth.
- Pregnancy complications: Many health conditions complicate pregnancy in advanced age women. This also increases the risk to the mother and the baby. It impacts the pregnancy outcome of an ICSI cycle.
The impact of a woman’s age on pregnancy is seen in all fertility treatments, including ICSI. If you are a woman aged over 35, then it is important that you consult a fertility specialist and discuss the impact of all these factors on your pregnancy planning.
The quality of the male and female gametes (sperm and egg) plays a very crucial role in any infertility treatment. The best quality sperms and eggs can fertilize better and produce good quality embryos. The embryos of best quality show better implantation rates and later better chances at having a healthy baby.
With poor quality gametes, fertilization rates are reduced, poor quality embryos are formed and, eventually poor pregnancy outcomes are seen. It is important that the quality of gametes is best when undergoing an ICSI treatment.
If a couple had to undergo ICSI because of fertility problems, the following points can be considered in future pregnancies:
- If more embryos are produced, they can be cryopreserved for future use.
- This gives the couple options to plan another pregnancy without having to undergo the whole treatment all over again.
- Later they can simply consult their fertility doctor, and plan the next embryo transfer.
- Optimizing your health condition before planning another pregnancy is important (described above).
- If previous ICSI was a failure, consider options suggested by your fertility doctor (described above).
It is important that you follow up with your infertility specialist when planning another pregnancy, if you had undergone ICSI previously.
No, there is no definite evidence that ICSI born babies have any long-term health impact. Studies have shown that ICSI born babies have similar rates of congenital conditions as from an IVF or a natural conception.