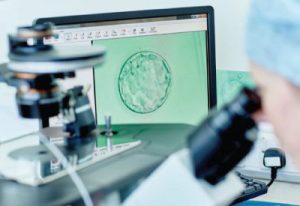

Does advance IVF technique actually increase the IVF success rate ? Or are they just a marketing gimmick and a way for IVF Clinics to charge more for an IVF Cycle.
The answer to this question is not so simple, like everything else in medicine. Let us talk about each of the advancement and try and figure out if they actually add on to IVF success rate.
The first Test Tube Baby in the world was born in the year 1978. After about four decades worth of various advancement in the field of ART, the success rate of an IVF Cycle has shown a significant improvement in terms of patient safety, take home baby rate and long term health of a baby born through IVF.
Blastocyst Culture
A Day 5 Embryo is called a Blastocyst. Over the years, Blastocyst Culture or extended culture has been a norm in any good IVF Lab. Any embryo that can progress to a Blastocyst by growing and multiplying it’s cells, is said to be robust enough to implant in a healthy uterus.
Usually only healthy embryos have a capability to reach a blastocyst stage. Culturing all fertilized oocytes till a Blastocyst stage can help the Embryologist identify the ones that will eventually lead to pregnancy. As many growing embryos easily reach Day 3 stage however only few of them have the potential to reach the Blastocyst stage.
It takes a very good embryo culture environment in the IVF Lab and the best of embryologists to culture embryos till Blastocyst stage with confidence. This is the reason why most good IVF Clinics charge extra for Blastocyst Culture.

Advantages of Blastocyst Culture:
- Reduces the Time to pregnancy by providing an opportunity to transfer the best grade blastocyst first.
- Reduces chance of twin pregnancy or multiple pregnancy by electively choosing single embryo transfer
- During fresh cycle, it gives two additional days to flush out the effects of medication provided during ovum pickup or ovarian stimulation.
- Blastocysts are more viable than Day 3 embryos, hence have better cryo-survivability meaning they can survive freezing and warming better than Day 3 embryos.
Having said this, there are certain instances, where Blastocyst transfer may not be beneficial, listed are a few of those cases:
- In case of 2 or less oocytes retrieved, the probability that both become a good blastocyst is very rare. In such a case, Day 3 transfer can be chosen.
- In cases of previous IVF failure where number of oocytes retrieved are less, and there has been failed Blastulation, it might make sense to transfer on Day 3 to see if the embryos perform any differently in vivo.
Laser Assisted Hatching (LAH)
IVF Clinics need a special instrument called a Laser to be able to burn the outer layer of the embryo called the zona pellucida. Not all patients will benefit from Laser Assisted hatching. The primary indication for Laser Assisted Hatching or LAH is thick zona pellucida on Day of Embryo Transfer (Day 3 or Day 5). Typically a Day 3 Embryo has thicker zona pellucida (outer shell) as compared to a Blastocyst, but all Day 3 Embryos do not need hatching. There are certain cases where the embryo shows thicker than normal zona, which necessitates the use of Laser prior to embryo transfer to maximize the chance of implantation.
IVF centres who predominantly perform Day 5 (Blastocyst) Transfer, seldom need LAH. This is because a Blastocyst expands and stretches and thins out the zona (outer covering). During this process the zona breaks at one or more points and results in the cells of Blastocyst to ooze out or hatch. Such hatching Blastocysts are called hatching blastocyst and are considered good for implantation.
However, at times, zona of some blastocysts are very thick and may impair the process of hatching. An Embryologist will apply a few laser shots to the zona of a Blastocyst at appropriate position. This creates a hole or opening on the zona allowing the process of hatching.
Does LAH improve the IVF success rate?
LAH cannot and should not be applied to all embryos. It should selectively be applied to embryos when needed. Many studies have indicated that for certain specific cases, Laser assisted hatching does improve the embryo implantation rate.
Timelapse Incubators
Timelapse incubators are special incubators with a camera attached to each incubator chamber that focuses a camera individually on each fertilized oocyte and provides timelapse growth images of an embryo. Whether or not timelapse incubator improve the IVF success rate is a highly debate-able topic.
Theoretically it does make sense to see the timelapse growth of each embryo without having to take them out of their culture environment, but many studies worldwide have failed to show any significant improvement in IVF success rate after comparing traditional benchtop incubators to timelapse incubators. One of the most important factors when it comes to Timelapse incubator is it’s huge cost. Hence it does not seem very practical to pay a substantial difference in IVF package just to culture in a Timelapse incubator when there does not seem any difference in IVF success rate.
As a patient, it is important to trust the IVF centre and choose the IVF Center where one has faith on the capabilities and knowledge of the Embryologist so that embryos are cultured in a good environment with minimal interventions even without a Timelapse incubator.

Pre implantation Genetic Testing for Aneuploidies ( PGT-A)
To know more about aneuploidies, please read our blog on chromosomal errors.
It is a known fact that genetic competency of oocytes decreases with age. A female aged between 35 to 39 will have as many as 40% of embryos that are genetically abnormal. However, with age the number of oocytes retrieved also reduces and when such reduced number of oocytes are left for Blastocyst Culture, only a few viable Blastocyst develops. It does not make sense to perform PGT-A for all Blastocyst always as it involves embryo biopsy which is an invasive test. During embryo biopsy few cells from the outer layer of Blastocyst (Trophectoderm) are sampled and tested to see the genetic competency of the blastocyst.
It is best to avoid any invasive test on the Blastocyst where possible, however one rule cannot apply to all and in certain cases like recurrent implantation failure, recurrent miscarriage, advanced maternal age or previous conception with aneuploidy errors, it does make sense to test the embryo before embryo transfer.
Does PGT Preimplantation Genetic Testing improve IVF success rate?
There are two types of genetic tests that can be performed on an embryo.
- PGT-A or testing for numerical chromosomal errors in embryo
- PGT-M or testing for monogenic error in embryo
PGT involves testing embryos created through IVF for either chromosomal abnormalities or specific genetic disorder before they are implanted into the uterus. PGT allows embryologists to select embryos that have the correct number of chromosomes or are free of specific genetic disease against which they have been tested. This is associated with a higher chance of successful implantation and a lower risk of pregnancy loss.
However, it’s important to note that PGT may not be necessary or appropriate for all couples undergoing IVF. PGT is typically recommended for couples with a history of recurrent pregnancy loss, advanced maternal age, or a known genetic disorder that increases the risk of chromosomal abnormalities. Your fertility specialist can help determine whether PGT is right for you and your partner based on your specific medical history and circumstances.
It makes sense to let your IVF specialist chose if you need to undergo PGT. One should refrain from unnecessarily testing just because it sounds fancy. Please chose an IVF specialist in Indore you trust and let the doctor decide if PGT is needed.
Does Ni-PGT or Non-invasive PGT improve IVF success Rate ?
Ni-PGT, or non-invasive preimplantation genetic testing, is a newer technique for assessing chromosomal status of an embryo without the need for an invasive biopsy procedure. Ni-PGT analyses the spent culture medium i.e. the culture medium around a Blastocyst and tests it for genetic material, rather than removing cells from the embryo itself.
While Ni-PGT is a promising technique, the evidence on whether it improves IVF success rates is currently limited. Some studies have suggested that Ni-PGT may be as accurate as traditional PGT methods, but more research is needed to confirm these findings and determine whether Ni-PGT actually leads to better IVF outcomes.
It’s important to note that not all fertility clinics offer Ni-PGT, and the technique may not be appropriate for all couples. Your fertility specialist can help determine whether Ni-PGT is right for you based on your specific medical history and circumstances.
Also at this point it is important to mention that the only good embryologists understand the fine nuances of how to maximize the chances of getting a correct ni-PGT result by timing the procedure appropriately, so make sure you choose the right and best IVF Clinic with experienced embryologist.

Sperm Microfluidics
Sperm microfluidics is a way of identifying better sperms. It uses microfluidic channels to sort and select high-quality sperm for use in IVF / ICSI. The channels within a sperm microfluidic chip are designed to mimic the natural female reproductive tract and allow sperm to swim through, with the healthier and more motile sperm being separated from the less healthy or less motile ones.
While the use of sperm microfluidics is still relatively new and more research is needed to fully understand its effectiveness, initial studies have shown promising results in improving IVF success rates. Many studies have also shown that sperm microfluidics can increase the chances of fertilization and implantation, and reduce the risk of chromosomal abnormalities in embryos. But some other studies have also shown that sperm microfluidics do not offer significant difference in fertilization and or implantation.
What is most paramount is to understand that no matter what technology is used, it cannot be a one size fits all and hence not all types of patients will benefit from use of sperm microfluidics. The best person to judge if a patient will benefit from this technology is an Embryologist, who can perform detailed assessment on patient’s semen analysis and decide if it makes sense to use sperm microfluidics for the patient. Make sure you choose and experienced embryologist who is well read and knows what is in best interest of patients.
Does PICSI or Physiological ICSI improve IVF success rate ?
PICSI, which stands for physiological intracytoplasmic sperm injection, is a laboratory technique used during in vitro fertilization (IVF) to select the best quality sperm for fertilization. It involves using a specialized dish containing hyaluronan, a substance that mimics the natural environment of the egg, to select mature and high-quality sperm for injection into the egg.
Studies have shown mixed results when it comes to the effectiveness of PICSI in improving IVF success rates. Some studies have reported a higher fertilization rate, better embryo quality, and improved pregnancy rates with the use of PICSI, while others have found no significant difference in IVF outcomes compared to traditional sperm selection techniques.
Overall, while PICSI may be a promising technique for improving IVF success rates, more research is needed to determine its efficacy and identify which patient populations may benefit most from its use. Ultimately, the decision to use PICSI during IVF should be made by the Embryologist on a case-by-case basis after consulting with a fertility specialist.
Does IMSI or Intracytoplasmic morphologically selected sperm injection improve IVF success rate ?
IMSI, which stands for intracytoplasmic morphologically selected sperm injection, is a laboratory technique used during in vitro fertilization (IVF) to select the best quality sperm for fertilization based on their morphology (shape and structure). It involves using a high-powered microscope to examine sperm in greater detail than is possible with conventional techniques.
Several studies have suggested that IMSI may improve IVF success rates, particularly in cases where male infertility is a factor. Some studies found that IMSI was associated with a significantly higher clinical pregnancy rate compared to conventional sperm selection techniques.
However, other studies have reported conflicting results, and more research is needed to confirm the effectiveness of IMSI in improving IVF outcomes. Additionally, IMSI is a more time-consuming and expensive technique than conventional sperm selection methods, so it may not be a viable option for all patients undergoing IVF.
Overall, while IMSI shows promise in improving IVF success rates, it should be used on a case-by-case basis and after consulting with a fertility specialist to determine the best course of treatment.

Does use of Artificial Intelligence Enhanced non-invasive PGT-A improve IVF success rate ?
AI can be used to predict the ploidy of embryos by analysing the morphological features of the embryos. Ploidy refers to the number of sets of chromosomes in an embryo and is an important factor in determining its viability and potential for implantation. Embryo morphology, or the physical appearance of the embryo, is a commonly used criterion for embryo selection in IVF.
The use of AI in morphological assessment of blastocyst can reduce the subjectivity and variability of manual embryo grading, as well as increase the speed and accuracy of the analysis. Additionally, the use of AI may lead to a reduction in the number of embryos transferred, which can reduce the risk of multiple pregnancies and their associated complications.
However, more research is needed to fully evaluate the effectiveness of AI-enhanced non-invasive PGT-A and to determine the optimal conditions for its use. Additionally, AI technology is still developing, and its use in clinical settings requires careful consideration of ethical and regulatory issues.